Items filtered by date: December 2021
What to Know About a Broken Toe
Trauma to the foot, especially the toes, can occur in many ways. Banging them, stubbing them, or dropping something on them are a few different ways this trauma can occur. Given the fact that toes are positioned in front of the feet, they typically sustain the brunt of such trauma. When trauma occurs to a toe, the result can be a painful break or fracture. Another type of trauma that can break a toe is repeated activity that places stress on the toe for prolonged periods of time.
Broken toes can be categorized as either minor or severe fractures. Symptoms of minor toe fractures include throbbing pain, swelling, bruising on the skin and toenail, and the inability to move the toe with ease. Severe toe fractures require medical attention and are indicated when the broken toe appears crooked or disfigured, when there is tingling or numbness in the toe, or when there is an open, bleeding wound present on the toe.
Generally, a minor toe break will heal without long-term complications. However, it is important to discontinue activities that put pressure on the toe. It is best to stay off of the injured toe and immediately get a splint or cast to prevent any more additional movement of the toe bones. You can also immobilize your toe by placing a small cotton ball between the injured toe and the toe beside it. Then, tape the two toes together with medical tape. Swelling can be alleviated by placing an ice pack on the broken toe directly as well as elevating your feet above your head.
Severe toe fractures may be treated with a splint, cast, and in some cases, minor surgery, especially when the big toe has been broken. Due to its position and the pressure the big toe endures with daily activity, future complications can occur if it is not properly treated. Pain associated with minor toe fractures can be managed with over-the-counter pain medications. Prescription pain killers may be necessary for severe toe fractures.
The healing time for a broken toe is approximately four to six weeks. In severe cases where the toe becomes infected or requires surgery, healing time can take up to eight weeks or more. While complications associated with a broken toe are immediately apparent, it is important to note that there are rare cases when additional complications, such as osteoarthritis, can develop over time. You should immediately speak with your podiatrist if you think you have broken your toe due to trauma. They will be able to diagnose the injury and recommend the appropriate treatment options.
What You Need to Know About Broken Toes
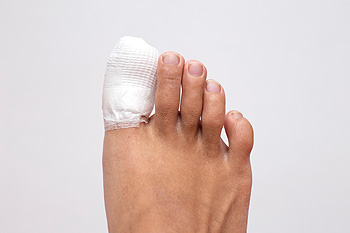 Broken toes often result from trauma. They may occur from dropping something directly on the toes, stubbing a toe, or bending them the wrong way. Toes can also break due to a stress fracture after a sudden increase in activity. The common indications of a broken toe include a snapping or popping sound at the time of the injury, swelling, bruising, and pain that becomes worse when the toe is moved. Patients who notice these symptoms may have a broken toe and would be wise to see a podiatrist who can assess the injury. A podiatrist will need to take an x-ray, and if a broken toe is confirmed, they can determine the best course for treatment. Depending on the nature of the break, the toe can be “buddy-taped” to the uninjured toe next to it, placed in a cast, or in severe cases surgery may be required.
Broken toes often result from trauma. They may occur from dropping something directly on the toes, stubbing a toe, or bending them the wrong way. Toes can also break due to a stress fracture after a sudden increase in activity. The common indications of a broken toe include a snapping or popping sound at the time of the injury, swelling, bruising, and pain that becomes worse when the toe is moved. Patients who notice these symptoms may have a broken toe and would be wise to see a podiatrist who can assess the injury. A podiatrist will need to take an x-ray, and if a broken toe is confirmed, they can determine the best course for treatment. Depending on the nature of the break, the toe can be “buddy-taped” to the uninjured toe next to it, placed in a cast, or in severe cases surgery may be required.
A broken toe can be very painful and lead to complications if not properly fixed. If you have any concerns about your feet, contact Dr. Tupper from Coshocton Foot Health Center. Our doctor will treat your foot and ankle needs.
What to Know About a Broken Toe
Although most people try to avoid foot trauma such as banging, stubbing, or dropping heavy objects on their feet, the unfortunate fact is that it is a common occurrence. Given the fact that toes are positioned in front of the feet, they typically sustain the brunt of such trauma. When trauma occurs to a toe, the result can be a painful break (fracture).
Symptoms of a Broken Toe
- Throbbing pain
- Swelling
- Bruising on the skin and toenail
- The inability to move the toe
- Toe appears crooked or disfigured
- Tingling or numbness in the toe
Generally, it is best to stay off of the injured toe with the affected foot elevated.
Severe toe fractures may be treated with a splint, cast, and in some cases, minor surgery. Due to its position and the pressure it endures with daily activity, future complications can occur if the big toe is not properly treated.
If you have any questions please feel free to contact our office located in Coshocton, OH . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Plantar Fasciitis
The plantar fascia is a connective tissue in the heel that stretches across the bottom length of your foot. Plantar fasciitis occurs when the connective tissue becomes inflamed, causing heel pain and discomfort during physical activity. Although the condition is completely treatable, traditional methods can take up to a year to start becoming effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding the condition is important for managing and treating it. One of the most common causes of plantar fasciitis is excessive running, especially with improper fitting or non-supportive shoes. Too much exercise can lead to the plantar fascia being overworked and overstretched, which can cause tears in the tissue. Along with improper fitting shoes, pronation, the rolling of the feet inward, is a common cause of plantar fasciitis. If not treated properly, the plantar fascia becomes overstretched and starts to tear, causing inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options. For less severe cases, conservative home remedies include taking anti-inflammatory drugs to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching and exercising your feet to re-strengthen the tissue, and using orthotic devices are all ways to help manage your plantar fasciitis.
For more severe cases, shockwave therapy has become a common solution for plantar fasciitis. Shockwave therapy can effectively break up the tissue on the bottom of your foot which facilitates healing and regeneration. This fights the chronic pain caused by plantar fasciitis. Even if this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be done to permanently correct the issue and stop the inflammation and pain in your heels.
No matter what the case may be, consulting your podiatrist is the first and best step to recovery. Even the slightest amount of heel pain could be the first stage of plantar fasciitis. Untreated symptoms can lead to the tearing and overstretching of tissue. Because the tearing of tissue can be compounded if it remains ignored, it can evolve into a severe case. The solution is early detection and early treatment. Talk to your podiatrist about the possibilities of plantar fasciitis if you’re experiencing heel pain.
The Possible Causes and Treatments of Plantar Fasciitis
The plantar fascia is a long, thick band of tissue that spans from the heel bone along the bottom of the foot to the toes. The plantar fascia supports the bottom of the feet and toes (as the heel rises) during walking, running, and jumping. The plantar fascia can become overly stressed or even tear or rupture from overuse or injury, causing pain and inflammation (plantar fasciitis). Being obese, standing/working on your feet for prolonged periods of time, having flat feet or high arches, and engaging in activities that involve dancing, marching or running can all contribute to, or worsen the symptoms of, plantar fasciitis. Wearing certain footwear, such as high heels, flip flops, worn out shoes, or other footwear with inadequate support, can also put you at an increased risk of developing this condition. A podiatrist will use a variety of treatment protocols to treat plantar fasciitis, depending upon the severity of the condition and how long the patient has been suffering from it. A combination of rest, icing, stretching, taping, protective footwear, orthotics, and pain medication may help heal the damage done to the plantar fascia and reduce pain and inflammation. A podiatrist may treat more severe or chronic plantar fasciitis (including cases that don’t respond to initial treatment) with steroid injections, laser therapy, or even surgery.
Plantar fasciitis is a common foot condition that is often caused by a strain injury. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Dr. Tupper from Coshocton Foot Health Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is a ligament that connects your heel to the front of your foot. When this ligament becomes inflamed, plantar fasciitis is the result. If you have plantar fasciitis you will have a stabbing pain that usually occurs with your first steps in the morning. As the day progresses and you walk around more, this pain will start to disappear, but it will return after long periods of standing or sitting.
What Causes Plantar Fasciitis?
- Excessive running
- Having high arches in your feet
- Other foot issues such as flat feet
- Pregnancy (due to the sudden weight gain)
- Being on your feet very often
There are some risk factors that may make you more likely to develop plantar fasciitis compared to others. The condition most commonly affects adults between the ages of 40 and 60. It also tends to affect people who are obese because the extra pounds result in extra stress being placed on the plantar fascia.
Prevention
- Take good care of your feet – Wear shoes that have good arch support and heel cushioning.
- Maintain a healthy weight
- If you are a runner, alternate running with other sports that won’t cause heel pain
There are a variety of treatment options available for plantar fasciitis along with the pain that accompanies it. Additionally, physical therapy is a very important component in the treatment process. It is important that you meet with your podiatrist to determine which treatment option is best for you.
If you have any questions, please feel free to contact our office located in Coshocton, OH . We offer the newest diagnostic and treatment technologies for all your foot care needs.
How to Get a Proper Shoe Fit
Many people suffer from foot problems because their shoes are poorly fitted. When shopping for a new pair of shoes, fashion usually triumphs over comfortability. A pair of well fitted shoes is essential in preventing foot problems and potential injuries.
Poorly fitted shoes can cause foot issues such as plantar fasciitis, bunions, hammertoes, ingrown toenails, and foot pain. Shoes such as high heels and sandals may cause problems for your feet. These shoes put the foot in an unnatural position for long periods and fail to provide good foot support. It is recommended to not wear either one for an extended period.
When you are trying on shoes, make sure they have enough space for your toes to move around. Shoes shouldn’t be cramped but also shouldn’t have too much room that your foot moves around in them. A snug shoe is a good choice. They should also provide good arch support and cushioning. Athletic shoes tend to offer both good support and cushioning. A degree of flexibility is necessary so they aren’t too stiff or too unsupportive.
If you can wear your shoes for a long period of time without experiencing any discomfort, this is a sign that your shoes fit properly. Do not be too dismayed if the shoe isn’t a perfect fit at first; many shoes take a few days to weeks to properly break in. However don’t expect an uncomfortable shoe to become fitted to your foot.
For those with foot conditions such as flat feet or pronation, orthotics may be helpful or even necessary to prevent foot pain. Orthotics are inserts that are placed in the shoe and provide support and cushioning for the foot. While there are many types of orthotics out there, custom-made orthotics may be necessary depending upon your foot and foot conditions.
Feet change in size over time. It is important to check your foot size over time so that you can make sure you have the perfect fit for your feet. A podiatrist can provide more information on proper shoe fitting and foot orthotics.
Conditions Caused by Poorly Fitting Shoes
 If you are wearing shoes that don’t fit correctly, you may not even notice. Wearing shoes that don’t fit correctly can lead to a variety of problems. Common foot-related issues that poorly fitted shoes can cause include plantar fasciitis (inflammation of the tendon that runs along the bottom of the foot), bunions (deformity of the big toe joint), blisters, corns, calluses and inflammation of the ball of the foot. Ways to ensure that your shoes fit correctly include making sure there is about a centimeter and a half between your toe and the edge of the shoe, checking that the ball of your foot is at the widest part of the shoe, and having your feet are measured by a professional. Anyone experiencing foot pain while wearing shoes may wish to consult with a podiatrist to be sure their shoes fit properly.
If you are wearing shoes that don’t fit correctly, you may not even notice. Wearing shoes that don’t fit correctly can lead to a variety of problems. Common foot-related issues that poorly fitted shoes can cause include plantar fasciitis (inflammation of the tendon that runs along the bottom of the foot), bunions (deformity of the big toe joint), blisters, corns, calluses and inflammation of the ball of the foot. Ways to ensure that your shoes fit correctly include making sure there is about a centimeter and a half between your toe and the edge of the shoe, checking that the ball of your foot is at the widest part of the shoe, and having your feet are measured by a professional. Anyone experiencing foot pain while wearing shoes may wish to consult with a podiatrist to be sure their shoes fit properly.
It is important to find shoes that fit you properly in order to avoid a variety of different foot problems. For more information about treatment, contact Dr. Tupper from Coshocton Foot Health Center. Our doctor will treat your foot and ankle needs.
Proper Shoe Fitting
Shoes have many different functions. They cushion our body weight, protect our feet, and allow us to safely play sports. You should always make sure that the shoes you wear fit you properly in order to avoid injuries and deformities such as: bunions, corns, calluses, hammertoes, plantar fasciitis, stress fractures, and more. It is important to note that although a certain pair of shoes might be a great fit for someone else, that doesn’t mean they will be a great fit for you. This is why you should always try on shoes before buying them to make sure they are worth the investment. Typically, shoes need to be replaced ever six months to one year of regular use.
Tips for Proper Shoe Fitting
- Select a shoe that is shaped like your foot
- Don’t buy shoes that fit too tight, expecting them to stretch to fit
- Make sure there is enough space (3/8” to ½”) for your longest toe at the end of each shoe when you are standing up
- Walk in the shoes to make sure they fit and feel right
- Don’t select shoes by the size marked inside the shoe, but by how the shoe fits your foot
The shoes you buy should always feel as good as they look. Shoes that fit properly will last longer, feel better, and improve your way of life each day.
If you have any questions, please feel free to contact our office located in Coshocton, OH . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Diabetic Foot Conditions
According to the American Diabetes Association (ADA), diabetes is a condition that affects approximately 23.6 million Americans. Around 750,000 new cases are diagnosed each year, and the disease’s most common form, Type 2 diabetes, makes up for 90 to 95 percent of these cases. Type 2 diabetes is especially prevalent among older Americans, those who are obese, and those who lead sedentary lifestyles.
Complications of the disease may lead to several foot and ankle-related conditions. The loss of nerve sensation, or neuropathy, can cause diabetics to lose feeling at the bottom of the feet and therefore leave them unaware of pain, pressure, and heat. Decreased circulation is another complication of diabetes that can slow down the healing of wounds and injuries; this can lead to the development of foot ulcers.
To prevent foot ulcers from forming, diabetics should examine their feet every day for small cuts and wear shoes that curtail pressure. Constant monitoring for the risk factors associated with ulcer formation can allow for early detection and therefore lessen the possibility of ulcers or, even worse, amputation. The removal of calluses and ingrown toenails should be left to the podiatrist to avoid improper removal and possible infection.
Diabetic patients may also experience foot deformities due to complications in their feet, such as limited joint mobility, muscle atrophy, and decreased fat padding. These complications can increase pressure in certain areas of the foot, which in turn can cause certain deformities, such as hammertoe, to form. Another deformity, Charcot foot, develops due to the collapsing of microfractures in the bones of the feet. The resulting deformity is a foot that is flattened and wider in appearance.
To help minimize pressure and prevent the development of these diabetes-related foot and ankle conditions, your podiatrist may consider using orthotics or special shoes. Charcot foot may be treated using walkers, custom orthotic insoles, or non-weight-bearing or rigid weight-bearing casts or braces. In more serious cases, surgery may be considered to treat more developed deformities. Ulcers can be further cared for with the help of proper diet, medication to control glucose, intensive wound care, and infection treatment.
The Importance of Foot Care for Diabetic Patients
 Patients who have diabetes may experience a variety of foot related complications, and in severe cases those complications can lead to amputation. Because diabetes can cause patients to lose sensation in their feet, noticing problems can become very difficult. Diabetes can cause poor blood flow, a slowdown of healing in wounds on the feet, and an increased numbness of the feet and toes. This is why establishing a foot-care action plan with a podiatrist, as well as scheduling regular checkups is suggested. Some things that can be implemented daily include checking for wounds or sores, washing and drying the feet thoroughly, and protecting the feet with properly fitting footwear. A podiatrist will also be able to help treat wounds on the feet, as well as provide guidance on shoes specifically designed for diabetic patients.
Patients who have diabetes may experience a variety of foot related complications, and in severe cases those complications can lead to amputation. Because diabetes can cause patients to lose sensation in their feet, noticing problems can become very difficult. Diabetes can cause poor blood flow, a slowdown of healing in wounds on the feet, and an increased numbness of the feet and toes. This is why establishing a foot-care action plan with a podiatrist, as well as scheduling regular checkups is suggested. Some things that can be implemented daily include checking for wounds or sores, washing and drying the feet thoroughly, and protecting the feet with properly fitting footwear. A podiatrist will also be able to help treat wounds on the feet, as well as provide guidance on shoes specifically designed for diabetic patients.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Dr. Tupper from Coshocton Foot Health Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact our office located in Coshocton, OH . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Read more about Diabetic Foot ConditionsArthritic Foot Care
During your lifetime, you will probably walk about 75,000 miles, which is quite a lot of stress to put on your feet. As you get older, the 26 bones and 30 joints in each of your feet will lose flexibility and elasticity. Your foot’s natural shock absorbers will wear down as well. Having arthritis added to this mix only makes matters worse. Your joints will become distorted and inflamed, which is why arthritic foot care needs to be something to think about every day.
When dealing with arthritis, having additional foot complications, such as bunions, hammertoes, or neuroma, can be a serious detriment. To avoid these, buy well-fitting shoes with a lower heel and good support. Arthritis causes you to lose your arch, so having shoes with good arch support is also highly recommended.
Aside from getting good arch support, the shoes need to fit comfortably and properly as well. A good place to start is by leaving a finger width between the back of the shoe and your foot to gauge proper size. It is also helpful to have a square or rounded toe box in the front to provide even more comfort. Another thing to look for is a rubber sole that can provide a cushion and absorb shock as you walk. This adds flexibility to the ball of your foot when you push off your heel to walk.
Exercise is another key aspect of arthritic foot care. Exercise not only strengthens and stretches your muscles and joints, but helps to prevent further injury and pain as well. Stretching the Achilles tendon, the tendon located in the back of your heel, will give you added mobility and reduce pain due to stress. Another thing you can do is massage your feet, kneading the ball of your foot as well as your toes from top to bottom.
Stretching the Achilles tendon is a simple exercise that you can do at home anytime. Lean against the wall with your palms flat against the surface while placing one foot forward, towards the wall, and one foot behind you. Bend your forward knee towards the wall while keeping your back knee locked straight, and make sure both your heels are completely touching the ground at all times. This will stretch your Achilles tendon and calf muscles as well. You will feel the stretch almost immediately. You can also stretch your toes in a couple ways. One involves taking a rubber band and wrapping it around both your big toes while your heels remain together. Then, pull them apart to stretch your big toe. You can also place a rubber band around all the toes of one of your feet. Then, try to separate each individual toe, stretching them all.
A final step you can take to help your arthritis is taking non-steroid, non-inflammatory drugs or topical medicines with capsaicin. Unfortunately, there is no complete way to remove all of your arthritic pain. However, following some of this advice can go a long way in staying as pain-free as possible.